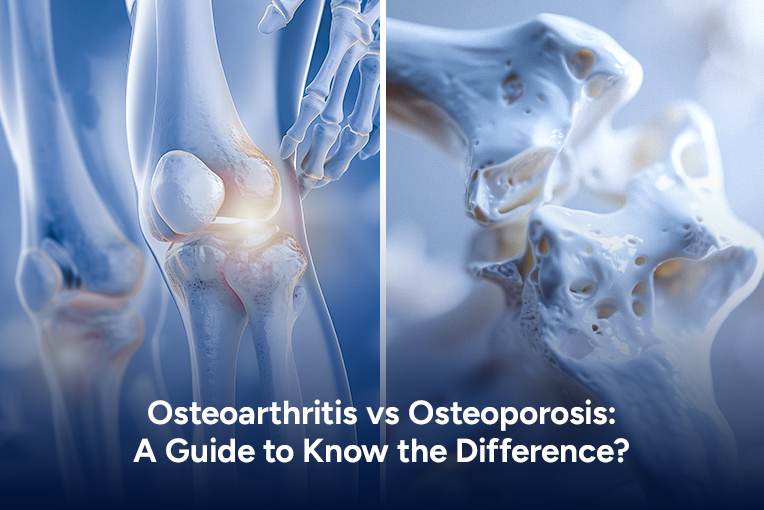
What is Rheumatology?
Expert Insights
Why the First Rheumatology Visit Feels So Detailed?
Rheumatology relies more on history than many specialties.
That’s because autoimmune and inflammatory conditions often leave subtle clues long before tests turn positive.
Spending time on your timeline isn’t inefficiency; it’s how missed diagnoses are avoided.
What Does a Rheumatologist Do?
- Diagnose inflammatory, autoimmune, and musculoskeletal disorders
- Differentiate mechanical strain, inflammation, autoimmunity, and nerve-related pain
- Use targeted testing (blood tests, imaging, sometimes joint fluid analysis) to narrow causes
- Build a treatment plan that can include medications, injections, physical therapy, lifestyle strategies, and follow-up monitoring
Clarity Starts with AZZ
Reasons When You Should See a Rheumatologist
- Joint pain lasting more than 6 weeks
- Pain in multiple joints at once
- Morning stiffness (especially if it lasts a long time)
- Swelling, warmth, or tenderness in joints
- Fatigue, generalized weakness, or systemic symptoms that don’t make sense yet
- A family history of autoimmune or rheumatic disease
- Abnormal inflammatory markers or antibody tests (your PCP may start this workup)
Your Checklist for First Rheumatology Appointment
- Symptom journal (dates, location, what makes it better/worse, morning vs evening, swelling, range-of-motion limits)
- Medication list (prescriptions, OTC meds, vitamins, supplements—include dose and how often)
- Past records (prior lab work, X-rays, MRI/CT reports, clinic notes—anything relevant)
- Family history (autoimmune disease, rheumatoid arthritis, lupus, gout, psoriasis, etc.)
- A short list of your top questions, in priority order
Your Story Matters
What to Wear to a Rheumatology Appointment
- Short sleeves or layers that roll up easily
- Pants you can move in
- Shoes that come off easily (foot/ankle checks are common)
- Avoid tight compression clothing if it limits exam access
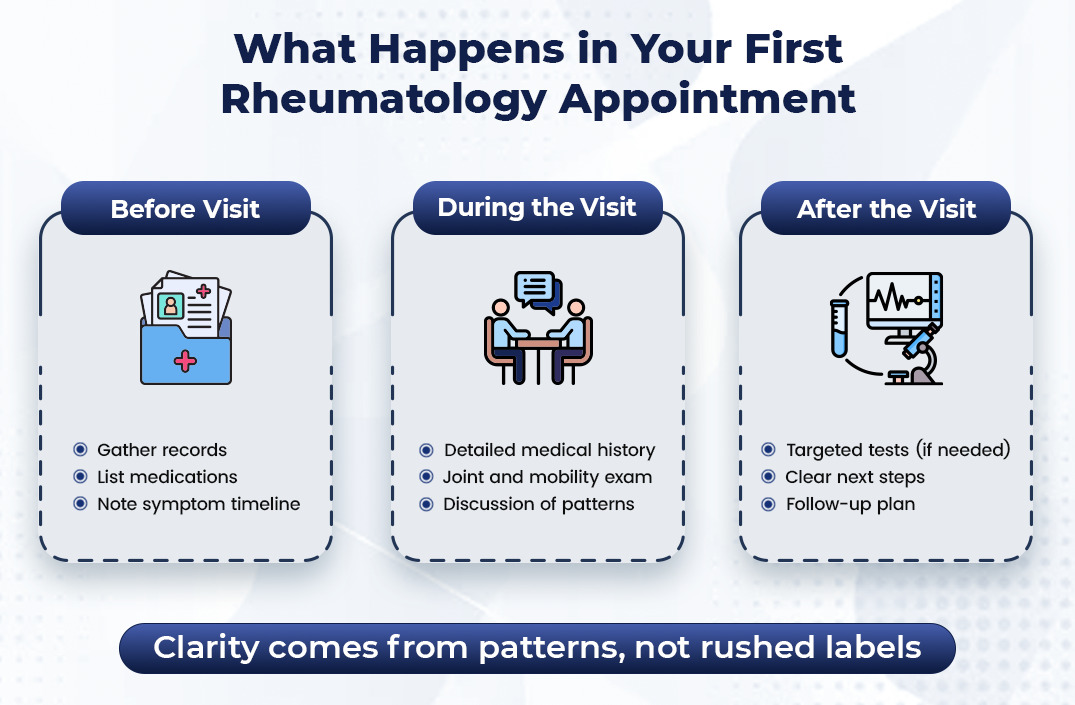
What Happens at Your First Rheumatology Appointment?
Step 1: A detailed history (the most important part)
- When did symptoms start, and how have they evolved?
- What’s worse in the morning? How long until you loosen up?
- Any swelling? Any redness or warmth?
- What makes symptoms better or worse (activity, rest, heat/cold, stress)?
- What other symptoms show up (rash, eye irritation, fevers, fatigue)?
- What have other doctors done so far, and what helped or didn’t?
Step 2: A joint and musculoskeletal exam
- Swelling, tenderness, warmth, redness
- Range of motion, mobility limits
- Patterns that suggest specific conditions (hands vs spine vs large joints, symmetrical vs one-sided)
Step 3: Planning tests (if needed)
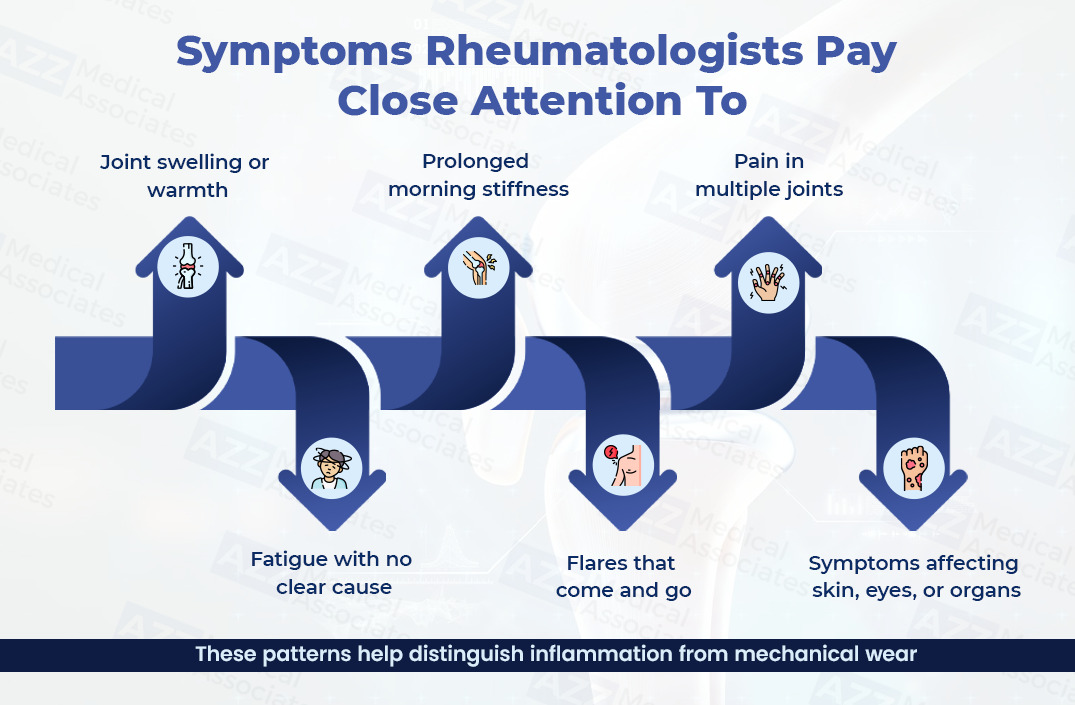
What Symptoms Does a Rheumatologist Look for?
- Pain with inflammation (swelling, warmth, prolonged stiffness)
- Symptoms across different tissues (joints plus skin, eyes, lungs, kidneys)
- Fatigue and systemic features
- Symptoms that move, spread, or flare in cycles
Tests You might Hear About
Blood tests (common examples)
- CRP and ESR (inflammation markers)
- Antibodies like rheumatoid factor, anti-CCP, or ANA (used in specific contexts)
- Sometimes, genetic markers like HLA-B27, depending on symptoms
- CBC, organ function tests, and other labs to rule in/out causes
Imaging
- An X-ray can show structural changes, though early disease may not show much
- Ultrasound can help detect early inflammatory changes in joints
- MRI or CT may be used in select cases when deeper detail is needed
Joint Fluid Analysis (when there’s significant swelling)
Not Every Answer Is Immediate
Why a Diagnosis Can Take Time (and what your doctor does in the meantime)
- Treat pain and inflammation to improve function
- Recommend activity adjustments, rest, and supportive therapies
- Plan next steps and follow-up timing
Why “Wait and Watch” Is Sometimes the Right Medical Decision
Why People Choose Us
- All insurance accepted
- 23+ locations across New Jersey
- Telehealth/virtual visits
- No wait time in appointments
- Appointments within 24 hours
- Weekend appointments
- Walk-in appointments
- Experienced Rheumatologists
- Chronic condition management
- In-house labs/diagnostics (where available)
- Medication management
- Follow-up care
- Evidence-based care
- Clear communication
Questions to ask Your Rheumatologist on Your First Visit
- What conditions are you considering, and why?
- What tests do I need, and what will they tell us?
- How and when will results be shared?
- What symptoms should prompt an earlier call?
- What are the treatment options if this is inflammatory arthritis?
- How often should I follow up?
What Happens After the First Visit
- A testing plan (if needed)
- A timeline for results and next steps
- A follow-up plan (especially if symptoms are progressing)
Quick Answers for Your Questions
- What kind of doctor treats arthritis? Often, a rheumatologist (an arthritis doctor called a rheumatologist) is consulted, especially when inflammation or autoimmune disease is suspected.
- How do you spell rheumatologist? Rheumatologist.
- What does a rheumatologist treat? Many inflammatory, autoimmune, and musculoskeletal conditions—not just rheumatoid arthritis.
- What will rheumatologists do on their first visit? A deep history, a focused exam, and a targeted diagnostic plan.
Closing Note
From Symptoms to Direction
FAQs
What Insurance Plans Does AZZ Accept?
We accept all insurance plans, including Medicare and Medicaid. If you do not see your plan listed on the AZZ Website, call us at 609-890-1050.
Do I need a diagnosis before seeing a rheumatologist?
No. Many patients are referred because the diagnosis is unclear. A rheumatologist’s role is to evaluate patterns over time and decide what fits and what doesn’t, rather than confirm something that’s already obvious.
Will I get a diagnosis at my first rheumatology visit?
Sometimes, but not always. Some conditions declare themselves clearly on day one; others require labs, imaging, or follow-up. Not having a diagnosis immediately doesn’t mean nothing is wrong; it often means your doctor is being careful and precise.
What should I bring if I’ve seen multiple doctors already?
Bring prior lab results, imaging reports, and medication history, even if you think they “didn’t help.” Knowing what’s already been ruled out prevents repeated testing and speeds up decision-making.
What symptoms should I mention even if they seem unrelated?
Fatigue, rashes, eye irritation, mouth ulcers, fevers, numbness, or weight changes matter. Rheumatology often connects symptoms that seem unrelated at first glance.
Can a rheumatologist help even if my tests come back normal?
Yes. Many inflammatory or autoimmune conditions can have normal labs early on. Rheumatologists rely on clinical patterns, not labs alone, to guide care.
What should prompt me to call the office sooner after my visit?
New joint swelling, sudden weakness, severe pain, fever, or neurological symptoms should be reported promptly. Your doctor will tell you exactly what changes matter for your situation.